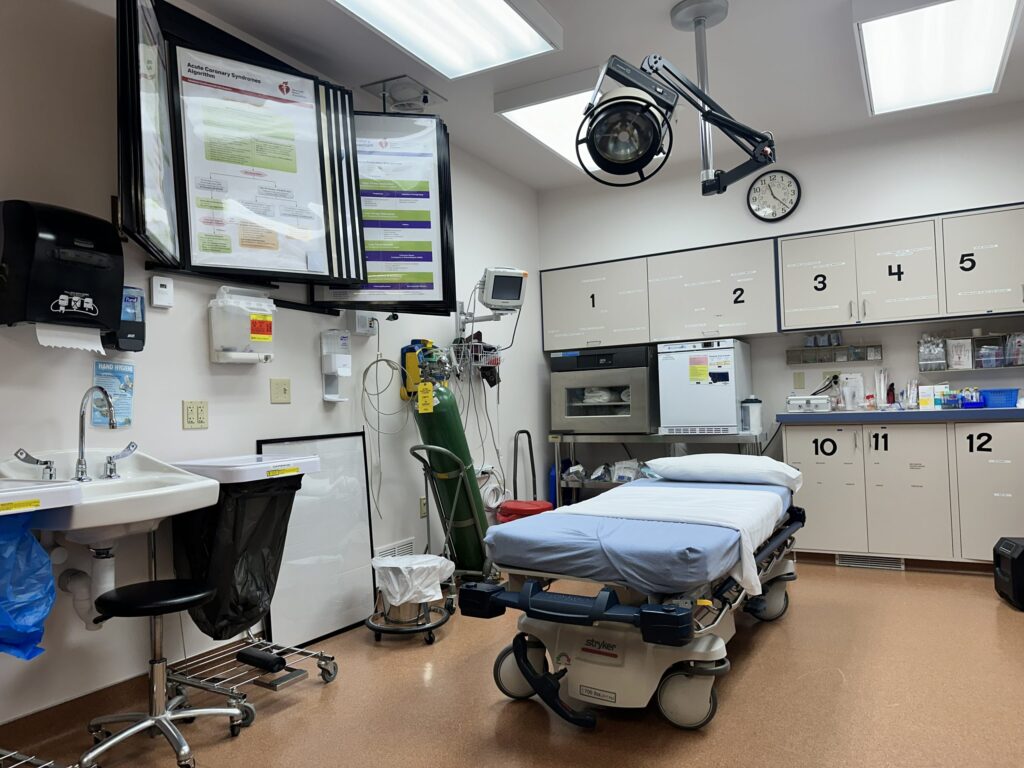
BIG SANDY — In Big Sandy, the medical center’s emergency department is just a single room with a curtain separating two beds. This rural hospital, with 25 beds, requires significant updates, according to former CEO Ron Wiens. Essential services are at risk as the facility faces at least $1 million in deferred maintenance costs.
Wiens, who recently vacated his CEO position, highlighted the hospital’s financial struggles, including a failing HVAC system. Built in 1965 by local farmers and ranchers, Big Sandy Medical Center began with nine beds. Today, donations and grants are essential to its survival.
Wiens hopes for support from Montana’s share of the $50 billion federal Rural Health Transformation Program. Although the state received over $233 million this year, this funding focuses on innovative health solutions, not direct service funding or hospital renovations. Montana’s leaders are concerned these projects might lead hospitals to reduce services while maintaining essential care.
The program was part of a legislative effort to mitigate expected Medicaid spending cuts of $1 trillion over the next decade. Montana’s application proposes initiatives like community gardens and mobile clinics to enhance rural health care. However, it also mentions rural hospitals “right-sizing” inpatient services, which may mean “downsizing” based on specific facility recommendations.
Shane Chauvet, a Big Sandy rancher, has firsthand experience with the medical center’s value. During a storm, a metal fragment nearly severed his arm, and the hospital’s emergency response was crucial. He fears service cutbacks could destabilize the hospital and the broader community.
Other states, like Wyoming and Oklahoma, also face potential service reductions. Wyoming officials interpret “right-sizing” as focusing on essential services while ensuring long-term financial stability. Some states may help hospitals transition to Rural Emergency Hospitals, which would eliminate inpatient services in favor of emergency and outpatient care.
Brock Slabach from the National Rural Health Association expressed concern that the funding might not reach its intended purpose. Cutting services, like labor and delivery, could drive people from rural towns, impacting patient numbers.
Despite apprehensions, some state health leaders remain optimistic. Ed Buttrey, CEO of the Montana Hospital Association, believes the state’s plan could help rural hospitals survive Medicaid cuts. Chauvet, reflecting on his near-death experience, now considers the local hospital essential for the community’s survival.
—
Read More Montana News