Article Summary –
The One Big Beautiful Bill Act, signed by President Trump in 2025, introduces significant changes to Medicaid, including new work requirements, increased out-of-pocket costs, and reduced state taxes on medical providers, potentially worsening health outcomes for 35.5 million Americans with kidney disease. The law, effective January 1, 2027, is particularly concerning for dialysis patients who must meet burdensome administrative requirements despite their medical conditions, and rural clinics may struggle due to reduced funding, exemplified by a Nebraska case where patients face long commutes for treatment. Additionally, for those above the poverty line, the act imposes a $35-per-treatment co-pay for dialysis, leading to over $5,000 in annual expenses, causing financial strain that may force patients to choose between essential needs like food and healthcare.
Experts warn that the One Big Beautiful Bill Act, signed by President Trump in 2025, could severely impact kidney patients across the U.S.
The budget law modifies Medicaid administration, introducing new out-of-pocket expenses and work requirements for beneficiaries, restricting state taxes on medical providers, and requiring recipients to renew eligibility biannually.
These changes may worsen outcomes for nearly 35.5 million Americans with kidney disease, including over half a million on dialysis, and 300,000 Medicaid recipients.
Dr. Jesse Roach, nephrologist and senior vice president at the National Kidney Foundation, stated, “The worst is yet to come, as new requirements start Jan. 1, 2027.”
Medicaid work requirements demand non-exempt able-bodied recipients aged 18-64 to engage in work, education, or volunteering for 80 hours monthly. Dialysis patients may qualify for exemptions but must consistently submit paperwork.
Roach emphasized, “Many could get waivers, but chronic illness makes regular paperwork burdensome.”
The Commonwealth Fund explained the law reduces provider taxes from 6% to about 3.5%, affecting state claims for federal Medicaid funds. This may severely impact rural dialysis clinics, Roach said.
“Rural clinics are vulnerable due to tight margins and fewer patients. Lower reimbursements threaten their survival,” Roach explained.
NPR recently reported patients in Chadron, Nebraska, face long drives or relocation after a dialysis clinic closure. Hay Springs resident Mark Pieper now travels 200 miles round trip for treatment.
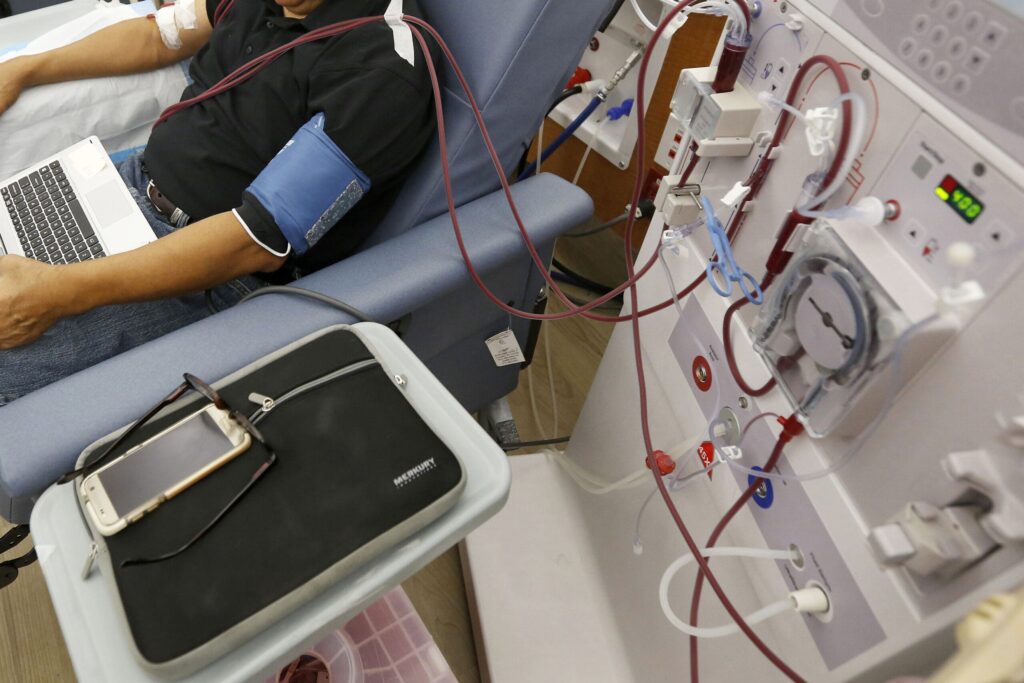
Hemodialysis patients follow a strict schedule, attending clinics three times a week for hours. The Mayo Clinic website details the process, noting fatigue as a common side effect. On off-days, patients manage medications and diet.
Peritoneal dialysis allows daily independence but involves infection risks and extensive training. It uses the abdomen lining to filter waste, as described by the Mayo Clinic.
Karol Franks, administrator of the “I Hate Dialysis” Facebook page and Living Donors Online, voiced concerns over Medicaid requirements for dialysis patients.
“Low-income, kidney failure patients face impossibilities like volunteering to qualify for Medicaid,” Franks said. She supports Medicaid for those able to work but highlights challenges for dialysis patients.
Her daughter began hemodialysis at 18, received a 2007 kidney transplant, switched to peritoneal dialysis in 2013, and had a second transplant in 2017.
Above-poverty patients face a $35 co-pay per dialysis treatment, totaling over $5,000 annually for thrice-weekly sessions.
“This financial burden forces critical choices between essential needs and health care,” Roach noted.
—
Read More Michigan News